
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Drug/Regimen
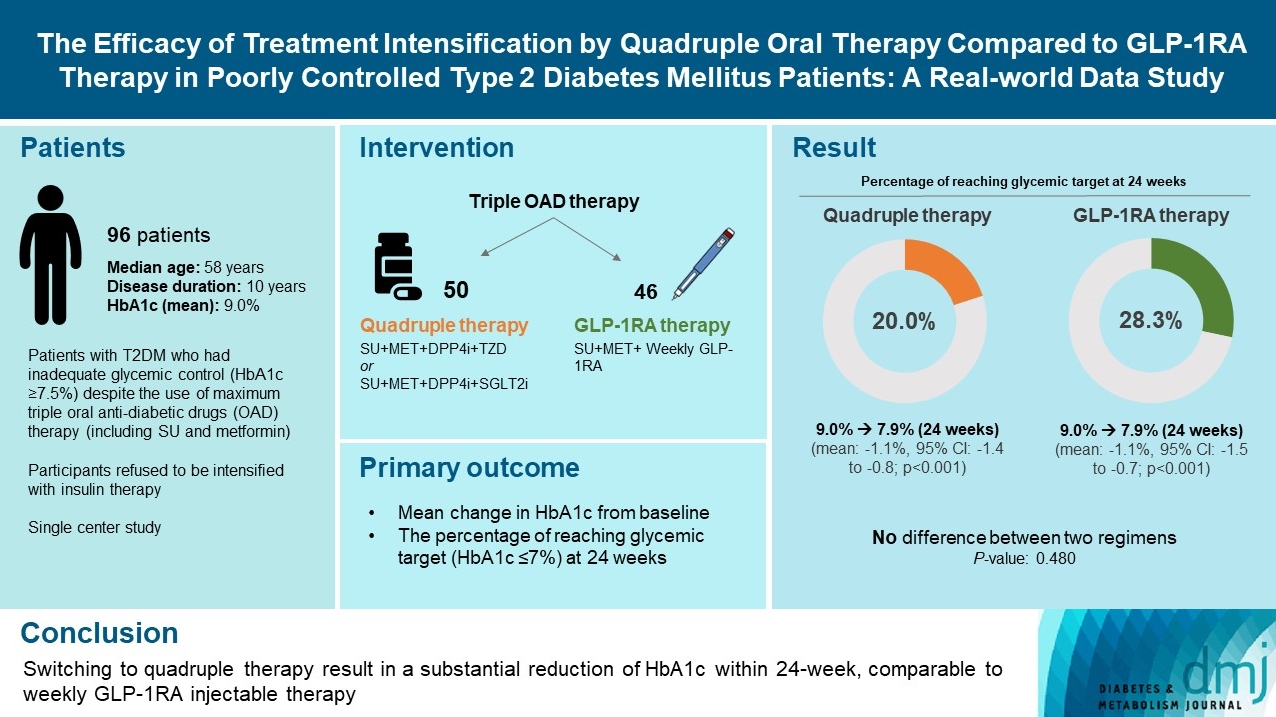
- The Efficacy of Treatment Intensification by Quadruple Oral Therapy Compared to GLP-1RA Therapy in Poorly Controlled Type 2 Diabetes Mellitus Patients: A Real-World Data Study
- Minyoung Kim, Hosu Kim, Kyong Young Kim, Soo Kyoung Kim, Junghwa Jung, Jong Ryeal Hahm, Jaehoon Jung, Jong Ha Baek
- Diabetes Metab J. 2023;47(1):135-139. Published online April 29, 2022
- DOI: https://doi.org/10.4093/dmj.2021.0373
- 7,547 View
- 296 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - We compared the glycemic efficacy of treatment intensification between quadruple oral antidiabetic drug therapy and once-weekly glucagon-like peptide-1 receptor agonist (GLP-1RA)-based triple therapy in patients with poorly controlled type 2 diabetes mellitus refractory to triple oral therapy. For 24 weeks, changes in glycosylated hemoglobin (HbA1c) from baseline were compared between the two treatment groups. Of all 96 patients, 50 patients were treated with quadruple therapy, and 46 were treated with GLP-1RA therapy. Reductions in HbA1c for 24 weeks were comparable (in both, 1.1% reduction from baseline; P=0.59). Meanwhile, lower C-peptide level was associated with a lower glucose-lowering response of GLP-1RA therapy (R=0.3, P=0.04) but not with quadruple therapy (R=–0.13, P=0.40). HbA1c reduction by GLP-1RA therapy was inferior to that by quadruple therapy in the low C-peptide subgroup (mean, –0.1% vs. –1.3%; P=0.04). Treatment intensification by switching to quadruple oral therapy showed similar glucose-lowering efficacy to weekly GLP-1RA-based triple therapy. Meanwhile, the therapeutic response was affected by C-peptide levels in the GLP-1RA therapy group but not in the quadruple therapy group.
- Others
- Comparison of Vildagliptin and Pioglitazone in Korean Patients with Type 2 Diabetes Inadequately Controlled with Metformin
- Jong Ho Kim, Sang Soo Kim, Hong Sun Baek, In Kyu Lee, Dong Jin Chung, Ho Sang Sohn, Hak Yeon Bae, Mi Kyung Kim, Jeong Hyun Park, Young Sik Choi, Young Il Kim, Jong Ryeal Hahm, Chang Won Lee, Sung Rae Jo, Mi Kyung Park, Kwang Jae Lee, In Joo Kim
- Diabetes Metab J. 2016;40(3):230-239. Published online April 5, 2016
- DOI: https://doi.org/10.4093/dmj.2016.40.3.230
- 5,205 View
- 48 Download
- 13 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background We compared the efficacies of vildagliptin (50 mg twice daily) relative to pioglitazone (15 mg once daily) as an add-on treatment to metformin for reducing glycosylated hemoglobin (HbA1c) levels in Korean patients with type 2 diabetes.
Methods The present study was a multicenter, randomized, active-controlled investigation comparing the effects of vildagliptin and pioglitazone in Korean patients receiving a stable dose of metformin but exhibiting inadequate glycemic control. Each patient underwent a 16-week treatment period with either vildagliptin or pioglitazone as an add-on treatment to metformin.
Results The mean changes in HbA1c levels from baseline were –0.94% in the vildagliptin group and –0.6% in the pioglitazone group and the difference between the treatments was below the non-inferiority margin of 0.3%. The mean changes in postprandial plasma glucose (PPG) levels were –60.2 mg/dL in the vildagliptin group and –38.2 mg/dL in the pioglitazone group and these values significantly differed (
P =0.040). There were significant decreases in the levels of total, low density lipoprotein, high density lipoprotein (HDL), and non-HDL cholesterol in the vildagliptin group but increases in the pioglitazone group. The mean change in body weight was –0.07 kg in the vildagliptin group and 0.69 kg in the pioglitazone group, which were also significantly different (P =0.002).Conclusion As an add-on to metformin, the efficacy of vildagliptin for the improvement of glycemic control is not inferior to that of pioglitazone in Korean patients with type 2 diabetes. In addition, add-on treatment with vildagliptin had beneficial effects on PPG levels, lipid profiles, and body weight compared to pioglitazone.
-
Citations
Citations to this article as recorded by- Factors contributing to the adverse drug reactions associated with the dipeptidyl peptidase-4 (DPP-4) inhibitors: A scoping review
Swetha R. Reghunath, Muhammed Rashid, Viji Pulikkel Chandran, Girish Thunga, K.N. Shivashankar, Leelavathi D. Acharya
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2023; 17(7): 102790. CrossRef - Efficacy and safety of evogliptin in patients with type 2 diabetes and non‐alcoholic fatty liver disease: A multicentre, double‐blind, randomized, comparative trial
Eugene Han, Ji Hye Huh, Eun Y. Lee, Ji C. Bae, Sung W. Chun, Sung H. Yu, Soo H. Kwak, Kyong S. Park, Byung‐Wan Lee
Diabetes, Obesity and Metabolism.2022; 24(4): 752. CrossRef - A double‐blind, Randomized controlled trial on glucose‐lowering EFfects and safety of adding 0.25 or 0.5 mg lobeglitazone in type 2 diabetes patients with INadequate control on metformin and dipeptidyl peptidase‐4 inhibitor therapy: REFIND study
Soree Ryang, Sang Soo Kim, Ji Cheol Bae, Ji Min Han, Su Kyoung Kwon, Young Il Kim, Il Seong Nam‐Goong, Eun Sook Kim, Mi‐kyung Kim, Chang Won Lee, Soyeon Yoo, Gwanpyo Koh, Min Jeong Kwon, Jeong Hyun Park, In Joo Kim
Diabetes, Obesity and Metabolism.2022; 24(9): 1800. CrossRef - The rs12617336 and rs17574 Dipeptidyl Peptidase-4 Polymorphisms Are Associated With Hypoalphalipoproteinemia and Dipeptidyl Peptidase-4 Serum Levels: A Case-Control Study of the Genetics of Atherosclerotic Disease (GEA) Cohort
Gilberto Vargas-Alarcón, María del Carmen González-Salazar, Christian Vázquez-Vázquez, Adrián Hernández-Díaz Couder, Fausto Sánchez-Muñoz, Juan Reyes-Barrera, Sergio A. Criales-Vera, Marco Sánchez-Guerra, Citlalli Osorio-Yáñez, Rosalinda Posadas-Sánchez
Frontiers in Genetics.2021;[Epub] CrossRef - Reduction in HbA1c with SGLT2 inhibitors vs. DPP-4 inhibitors as add-ons to metformin monotherapy according to baseline HbA1c: A systematic review of randomized controlled trials
A.J. Scheen
Diabetes & Metabolism.2020; 46(3): 186. CrossRef - Combination Therapy of Oral Hypoglycemic Agents in Patients with Type 2 Diabetes Mellitus
Min Kyong Moon
The Journal of Korean Diabetes.2018; 19(1): 23. CrossRef - Comparative Cardiovascular Risks of Dipeptidyl Peptidase-4 Inhibitors: Analyses of Real-world Data in Korea
Kyoung Hwa Ha, Bongseong Kim, Hae Sol Shin, Jinhee Lee, Hansol Choi, Hyeon Chang Kim, Dae Jung Kim
Korean Circulation Journal.2018; 48(5): 395. CrossRef - Safety and efficacy of low dose pioglitazone compared with standard dose pioglitazone in type 2 diabetes with chronic kidney disease: A randomized controlled trial
Bancha Satirapoj, Khanin Watanakijthavonkul, Ouppatham Supasyndh, Stephen L Atkin
PLOS ONE.2018; 13(10): e0206722. CrossRef - Combination therapy of oral hypoglycemic agents in patients with type 2 diabetes mellitus
Min Kyong Moon, Kyu Yeon Hur, Seung-Hyun Ko, Seok-O Park, Byung-Wan Lee, Jin Hwa Kim, Sang Youl Rhee, Hyun Jin Kim, Kyung Mook Choi, Nan-Hee Kim
The Korean Journal of Internal Medicine.2017; 32(6): 974. CrossRef - Combination Therapy of Oral Hypoglycemic Agents in Patients with Type 2 Diabetes Mellitus
Min Kyong Moon, Kyu-Yeon Hur, Seung-Hyun Ko, Seok-O Park, Byung-Wan Lee, Jin Hwa Kim, Sang Youl Rhee, Hyun Jin Kim, Kyung Mook Choi, Nan-Hee Kim
Diabetes & Metabolism Journal.2017; 41(5): 357. CrossRef - Efficacy and safety of adding evogliptin versus sitagliptin for metformin‐treated patients with type 2 diabetes: A 24‐week randomized, controlled trial with open label extension
Sang‐Mo Hong, Cheol‐Young Park, Dong‐Min Hwang, Kyung Ah Han, Chang Beom Lee, Choon Hee Chung, Kun‐Ho Yoon, Ji‐Oh Mok, Kyong Soo Park, Sung‐Woo Park
Diabetes, Obesity and Metabolism.2017; 19(5): 654. CrossRef - Antihyperglycemic agent therapy for adult patients with type 2 diabetes mellitus 2017: a position statement of the Korean Diabetes Association
Seung-Hyun Ko, Kyu-Yeon Hur, Sang Youl Rhee, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Hyun Jin Kim, Kyung Mook Choi, Jin Hwa Kim
The Korean Journal of Internal Medicine.2017; 32(6): 947. CrossRef - Antihyperglycemic Agent Therapy for Adult Patients with Type 2 Diabetes Mellitus 2017: A Position Statement of the Korean Diabetes Association
Seung-Hyun Ko, Kyu-Yeon Hur, Sang Youl Rhee, Nan-Hee Kim, Min Kyong Moon, Seok-O Park, Byung-Wan Lee, Hyun Jin Kim, Kyung Mook Choi, Jin Hwa Kim
Diabetes & Metabolism Journal.2017; 41(5): 337. CrossRef
- Factors contributing to the adverse drug reactions associated with the dipeptidyl peptidase-4 (DPP-4) inhibitors: A scoping review
- Clinical Significance of the Presence of Autonomic and Vestibular Dysfunction in Diabetic Patients with Peripheral Neuropathy
- Soo Kyoung Kim, Kyeong Ju Lee, Jong Ryeal Hahm, Sang Min Lee, Tae Sik Jung, Jung Hwa Jung, Sungsu Kim, Deok Ryong Kim, Seong-Ki Ahn, Won-Hee Choi, Soon Il Chung
- Diabetes Metab J. 2012;36(1):64-69. Published online February 17, 2012
- DOI: https://doi.org/10.4093/dmj.2012.36.1.64
- 3,852 View
- 46 Download
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background We investigated the prevalence of diabetic autonomic neuropathy (DAN) and vestibular dysfunction (VD) in diabetic patients with peripheral neuropathy.
Methods Thirty-five diabetic patients with peripheral neuropathy were enrolled from August 2008 to July 2009. All subjects underwent autonomic function tests. Nineteen of the patients (54.3%) underwent videonystagmography.
Results Diabetic autonomic neuropathy was observed in 28 patients (80%). A mild degree of autonomic failure was observed in 18 patients (64.3%), and a moderate degree of autonomic failure was observed in ten patients (35.7%). Factors related to DAN included diabetic nephropathy (
P =0.032), degree of chronic kidney disease (P =0.003), and duration of diabetes (P =0.044). Vestibular dysfunction was observed in 11 of 19 patients (57.9%). There was no significant association between DAN and VD.Conclusion Diabetic autonomic neuropathy was observed in 28 diabetic patients (80%) with peripheral neuropathy. Vestibular dysfunction was observed in nearly 60% of diabetic patients with peripheral neuropathy who complained of dizziness but showed no significant association with DAN. Diabetic patients who complained of dizziness need to examine both autonomic function and vestibular function.
-
Citations
Citations to this article as recorded by- β-Glucans obtained from fungus for wound healing: A review
Chunhua Xu, Fengxia Wang, Shibing Guan, Lizhen Wang
Carbohydrate Polymers.2024; 327: 121662. CrossRef - Dynamic and static balance functions in hemodialysis patients and non‐dialysis dependent CKD patients
Nobuyuki Shirai, Suguru Yamamoto, Yutaka Osawa, Atsuhiro Tsubaki, Shinichiro Morishita, Ichiei Narita
Therapeutic Apheresis and Dialysis.2023; 27(3): 412. CrossRef - Micro (mi) RNA and Diabetic Retinopathy
Sadashiv, Praveen Sharma, Shailendra Dwivedi, Sunita Tiwari, Pankaj Kumar Singh, Amit Pal, Sandeep Kumar
Indian Journal of Clinical Biochemistry.2022; 37(3): 267. CrossRef - Physiotherapists’ Perspectives on Type 2 Diabetes Management and as a Primary Condition for Referral to Physiotherapy Services: A Qualitative Descriptive Study
Sarah M. Janssen, Denise M. Connelly, Heather Gillis
Physiotherapy Canada.2022;[Epub] CrossRef - Subclinical vestibular dysfunction in type 1 diabetes mellitus
Abdollah Moossavi, Moslem Shaabani, Ensieh Nasli Esfahani, Mohsen Vahedi, Zakaria Enayati
Hearing, Balance and Communication.2021; 19(2): 86. CrossRef Potential Applications of Nanomaterials and Technology for Diabetic Wound Healing
Que Bai, Kai Han, Kai Dong, Caiyun Zheng, Yanni Zhang, Qianfa Long, Tingli Lu
International Journal of Nanomedicine.2020; Volume 15: 9717. CrossRef- Recent advancements in biopolymer and metal nanoparticle-based materials in diabetic wound healing management
Veena Vijayakumar, Sushanta K. Samal, Smita Mohanty, Sanjay K. Nayak
International Journal of Biological Macromolecules.2019; 122: 137. CrossRef - Auditory function and motor proficiency in type 1 diabetic children: A case-control study
Jalali Mir Mohammad, Soleimani Robabeh, Koohmanai Shahin, Tizno Saeed, Akbari Maryam
International Journal of Pediatric Otorhinolaryngology.2018; 109: 7. CrossRef - Vestibular profile of type 1 versus type 2 chronic diabetes mellitus
Ola Abdallah Ibraheem, Mohammad Ramadan Hassaan, Mayada Mohamed Mousa
Hearing, Balance and Communication.2017; 15(3): 133. CrossRef - Glycemic variability is an important risk factor for cardiovascular autonomic neuropathy in newly diagnosed type 2 diabetic patients
Wen Xu, Yanhua Zhu, Xubin Yang, Hongrong Deng, Jinhua Yan, Shaoda Lin, Huazhang Yang, Hong Chen, Jianping Weng
International Journal of Cardiology.2016; 215: 263. CrossRef - Impact of Diabetic Complications on Balance and Falls: Contribution of the Vestibular System
Linda J. D'Silva, James Lin, Hinrich Staecker, Susan L. Whitney, Patricia M. Kluding
Physical Therapy.2016; 96(3): 400. CrossRef - Shedding light on miR-26a: Another key regulator of angiogenesis in diabetic wound healing
Carlos Zgheib, Kenneth W. Liechty
Journal of Molecular and Cellular Cardiology.2016; 92: 203. CrossRef - Augmented asymmetrical visual field dependence in asymptomatic diabetics: Evidence of subclinical asymmetrical bilateral vestibular dysfunction
Rima Abdul Razzak, Jeffery Bagust, Sharon Docherty, Wiam Hussein, Abdullah Al-Otaibi
Journal of Diabetes and its Complications.2015; 29(1): 68. CrossRef - Associations between autonomic dysfunction and pain in chemotherapy‐induced polyneuropathy
H. Nahman‐Averbuch, Y. Granovsky, E. Sprecher, M. Steiner, T. Tzuk‐Shina, D. Pud, D. Yarnitsky
European Journal of Pain.2014; 18(1): 47. CrossRef - Balance training in the intervention of fall risk in elderly with diabetic peripheral neuropathy: A review
Xi Pan, Jiao-jiao Bai
International Journal of Nursing Sciences.2014; 1(4): 441. CrossRef - Synkope aus der Sicht des Neurologen
A. Bickel, J. Röther
Herz.2014; 39(4): 443. CrossRef - The Role of MicroRNAs in Diabetic Complications—Special Emphasis on Wound Healing
João Moura, Elisabet Børsheim, Eugenia Carvalho
Genes.2014; 5(4): 926. CrossRef - Recent advances on the development of wound dressings for diabetic foot ulcer treatment—A review
Liane I.F. Moura, Ana M.A. Dias, Eugénia Carvalho, Hermínio C. de Sousa
Acta Biomaterialia.2013; 9(7): 7093. CrossRef
- β-Glucans obtained from fungus for wound healing: A review
- The Classification of Diabetic Patients Presenting Diabetic Ketoacidosis: The Characteristics of Fulminant Type 1 Diabetes.
- Tae Sik Jung, Jong Ryeal Hahm, Jung Hwa Jung, Soon Il Chung
- Korean Diabetes J. 2008;32(6):534-536. Published online December 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.6.534
- 1,886 View
- 23 Download
- 1 Crossref
- A Case of Newly Diagnosed Type 2 Diabetes Mellitus Presenting with Rhinocerebral Mucormycosis.
- Jung Hwa Jung, Jong Ryeal Hahm, Mi Yeon Kang, Sung Won Moon, Tae Sik Jung, Deok Ryong Kim, Soon Il Chung
- Korean Diabetes J. 2004;28(3):225-230. Published online June 1, 2004
- 1,014 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - Rhinocerebral mucormycosis(RM) is a rare opportunistic fungal infection that mainly occurs in immunocompromised or diabetic patients, but rarely in healthy indi-viduals. This fungal infection usually begins at the nose and progresses through the paranasal sinuses, and secondarily invading the orbit and central nervous system. Because of its rapid progression and high mortality, early diagnosis and treatment are crucial to increase the patient survival rate. A combination of ampho-tericin B administration and surgery is a standard repertoire of RM treatment. Herein, a case in which a 69-year-old male patient with type 2 diabetes mellitus, presentings as RM, is reported. This patient had never been diagnosed with diabetes mellitus until the diabetes and RM were identified by us using the oral glucose tolerance test, measurement of the glycated hemoglobin level and a paranasal sinus CT scan. The RM was further confirmed by a biopsy of an oral mucosal ulcerative lesion. This case suggests that RM can present in newly diagnosed type 2 diabetes patients.
- The Appropriteness of New ADA Diagnostin Criteria for Diabetes Mellitus in Korean Population.
- Moon kyu Lee, Myung Shik Lee, Young Ki Min, Sung Hoon Kim, Byoung Joon Kim, Dong Jun Kim, Jong Ryeal Hahm, Eun Young Oh, Yun Jae Chung, Kyoung Ah Kim, Jae Hoon Chung, Kwang Won Kim
- Korean Diabetes J. 1999;23(3):336-351. Published online January 1, 2001
- 1,470 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The ADA has proposed a new diagnostic criteria for diabetes based on fasting plasma glucose, redefining diabetes as fasting plasma glucose 7.0 mmol/L. Since only a few studies for the appropriateness of tbis new ADA criteria were undertaken in the Korean population, we examined the appropriateness of the new ADA criteria by analyzing the results of oral glucose tolerance tests done in our hospital. METHODS: 507 oral glucose tolerance tests were conducted. Cases with diabetes and diseases that could affect the glucose tolerance were excluded. Plasma glucose was measured by the hexokinase method. Three groups of NGT, IGT, and DM by the WHO criteria of 2 hour-plasma glucose were redivided at each level of fasting plasma glucose. We calculated the sensitivity and specificity of each level of fasting plasma glucose (FPG), and the FPG value of maximum accuracy to diagnose diabetes with reference to the WHO criteria of 2 hour-plasma glucose. RESULTS: Correlation between the levels of fasting plasma glucose and 2 hour-plasma glucose was relatively low (r=0.676). FPG of 7.0 mmol/L for diagnosing diabetes was relatively specific (specificity=0.934), but not sensitive (sensitivity= 0.552). FPG value of maximum accuracy for diagnosing diabetes was 6.8 mmol/L. 39 % of IFG (> 6.1mmol/L and < 7.0mmol/L) was reclassified as diabetes by the criteria of 2 hour plasma glucose 11.1 mmol/L and 34 % of NFG (<6.1mmol/L) was reclassified as impaired glucose tolerance by the criteria of 2 hour plasma glucose > 7.8 mmol/L. CONCLUSION: The fasting plasma glucose of 7.0 mmol/L was relatively specific for diagnosing diabetes. However, the new ADA criteria tended to underestimate the prevalence of diabetes and impaired glucose tolerance in the Korean population. Therefore, oral glucose tolerance test may be needed to diagnose diabetes in high risk subjects. Large-scale cross-sectional and prospective studies will be needed to clarify these points.
- Measurement of Anti-Phogrin Antibody in Korean Autoimmune Deabetes; Comparison to Anti-IA-2 Antibody.
- Moon kyu Lee, Yong Ki Min, Myung Shik Lee, Sung Hoon Kim, Byoung Joon Kim, Dong Jun Kim, Jong Ryeal Hahm, Dong Kyu Jin, Kyoung Ah Kim, Kwang Won Kim
- Korean Diabetes J. 1999;23(3):269-277. Published online January 1, 2001
- 1,273 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Since the discovery of IA-2 as a major autoantigen in type 1 diabetes, the question arose as to whether other PTPs (protein tyrosine phosphatases) could act as diabetic autoantigens as well. A novel PTP, designated IA-2 B (phogrin; phosphatase homologue in granules of insulinoma) was isolated that has a high sequence similarity to IA-2. Since some studies suggested that auto- immunity to phogrin, rather than IA-2 may be more closely associated with the development of type 1 diabetes, we measured the frequency of anti-phogrin antibody in Korean patients with type 1 diabetes and compared it with that of anti-IA-2 antibody/ anti-GAD antibody. METHODS: The anti-phogrin antibody and the anti-IA-2 antibody were measured by radioligand binding assays using in vitro transcribed and translated S-labeled phogrin and IA-2, respectively. Anti-GAD antibody was measured using a commercial radioimmunoassay kit (RSR, Cardiff, U.K.). The subjects in this study consisted of 41 patients with classical type 1 diabetes, 22 with slowly progressive type 1 diabetes, and 39 with type 2 diabetes. Their average mean age was 16.9 years, 37.9 years and 45.3 years respectively. RESULTS: The prevalence of anti-phogrin antibody, anti-IA-2 antibody and anti-GAD antibody in classical type 1 diabetes was 24.4%, 26.8% and 51.2% respectively. That, in slowly progressive type 1 diabetes was 0%, 9.1% and 40.9% respectively. When the anti-GAD antibody assay and the anti-IA-2 antibody assay were combined, the prevalence of autoantibodies was 58.5% in classical type 1 diabetes and 50% in slowly progressive type I diabetes. However, the addition of the anti-phogrin antibody to the anti-GAD antibody/anti-IA-2 antibody measurement did not significantly increase the prevalence of autoantibody. The level of the antiphogrin antibody was positively correlated with that of the anti-IA-2 antibody. The presence of the anti-phogrin antibody and the anti-IA-2 antibody was negatively correlated with the age at diagnosis. One patient with type 1 diabetes had the anti-phogrin antibody without the anti-IA-2 antibody. CONCLUSION: Combined measurement of the anti-phogrin antibody with the anti-IA-2 antibody/ anti-GAD antibody did not significantly increase the prevalence of autoantibodies in Korean patients with type 1 diabetes. In the majority of Korean type 1 diabetes patients, the anti-phogrin antibody appears to share epitopes with the anti-IA-2 antibody. However, a small proportion of type 1 diabetes patients may have a specific autoimmune response to phogrin.
- The Significance of thebeta3 Adrenergic Receptor Gene Polymorphism in Obese Koreans.
- Byoung Joon Kim, Sung Hoon Kim, Dong Jun Kim, Jong Ryeal Hahm, Jin Seok Kim, Kyu Jeung Ahn, Jae Hoon Chung, Yong Ki Min, Myung Shik Lee, Moon Kyu Lee, Kwang Won Kim
- Korean Diabetes J. 1998;22(4):450-456. Published online January 1, 2001
- 1,323 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The b3 adrenergic receptor (b3-AR), expressed mainly in visceral fat of human, is involved in regulation of lipolysis and thermogenesis. The missense mutation of b3-AR gene, resulting in the replacement of tryptophan by arginine at position 64 (Trp64Arg), is associated with decreased resting metabolic rate, weight gain and development of obesity. The purpose of this study was to investigate the frequency of the b3-AR gene polymorphism in obese Koreans. Subjects and METHODS: b3-AR genotype was determined in 87 healthy Koreans who visited SMC for the purpose of health checking from Dec/1996 to Feb/1997. Oral glucose tolerance test was performed with 75 g glucose. Lipid profiles, insulin, C-peptide were measured. Anthropometric data was obtained from physical examination and medical records. The subjects with previously diagnosed diabetes mellitus, other endocrine diseases or chronic illness were excluded. To determine the polymorphism, genomic DNA was isolated and PCR and RFLP by MvaI were carried. RESULTS: 1. The difference in frequency of Trp64Arg mutation between two groups was highly significant. (12 subjects (63%) in obese group and 21 subjects (30%) in non obese group, p<0.02) 2. There was significantly high allele frequency in obese group. (obese group: 32 %; non obese group: 15 %, p<0.02). 3. According to BMI, there were significantly high WHR (0.88+0.04 vs 0.83+0.06,p=0.01), total body fat (29.8+7.4 vs 24.4+6.5%, p=0.01) and systolic blood pressure(132+19 vs 124+14mmHg, p=0.04) in obese group. 4. According to b3-AR genotype, there were significantly high WHR (0.830.056 vs. 0.860.05) and 120 min (260.5+171. 5 vs 355.9+234.6 pmol/L, p=0.04) insulin level during OGTT in heterozygote group. CONCLUSION: These results suggest that the frequency of the b3-AR gene mutation was significantly higher in obese Koreans and b3-AR gene polymorphism might play a role in the pathogenesis of obesity.

 KDA
KDA
 First
First Prev
Prev





